Was Dr. Centor right about Strep Throat?
Do the Centor criteria hold up to modern research standards?
“My throat hurts,” said every kid at some point in their young lives. If it is your kid with a sore throat, knowing how miserable it can be, you want to do something for them. But what?
Pharyngitis, or inflammation of the pharynx, can be caused by either a virus or a bacteria. The former requires supportive care while the latter needs antibiotics. So, can we differentiate the two?
Dr. Richard Centor was a new internal medicine residency grad who wanted to find out. In 1979 he embarked on a study that would morph the next 45+ years of sore throat management. He studied 286 adults who presented to the Medical College of Virginia emergency department with a sore throat. All throats were swabbed and each subject was asked about their symptoms, as well as signs such as fever over 101, presence of exudate, tonsil swelling, and swollen and tender anterior cervical lymph nodes. They found that if the patient had none of these 4 criteria, it was unlikely to be caused by a bacteria (Group A Streptococcus), but if they had all 4, the probability of a positive culture was 55%. In other words, if all 4 criteria are met, it is on par with a coin flip.
If they’re all negative, then there is a 3/100 chance it is still strep throat (Figure 1).

A large study of CVS minute clinics did find similar results to Dr. Centor’s initial study, but the question is: does it help us decide if antibiotics are needed? In this exceptionally large study, 7% of patients with a Centor Score of 0 still tested positive for Group A Strep. For patients with a score of 1-3, the basket in which most patients fall into that are sick enough to go to the doctor, the test was positive 12 to 38% of the time. And with the highest possible score, only 57% of the samples grew strep, meaning 43% of them were likely viral.
While these studies do have an impressive negative predictive value if all criteria are negative, it strikes me as suspicious that such non-specific criteria common to all infections could somehow be specific to bacterial ones. Since the 1981 publication, many large studies have failed to confirm these results.
For example, a study of 441 kids found no correlation between Centor score and Group A strep infection, reporting a high prevalence of Group A strep in kids with a score below 2, concluding that their results “confirm the ineffectiveness of Centor criteria as a predicting factor for the presence of Group A strep.” This was also true in this study of 0 to 3-year-olds in Finland or in this study of kids 3 to 12 where the authors determined that group A strep pharyngitis cannot be differentiated clinically. This was also the conclusion found of a systematic review from 2012 which looked at 34 studies and failed to find any useful prediction rule that could either rule in or rule out strep pharyngitis, or this systematic review that found these criteria are not sensitive or specific enough to be useful:
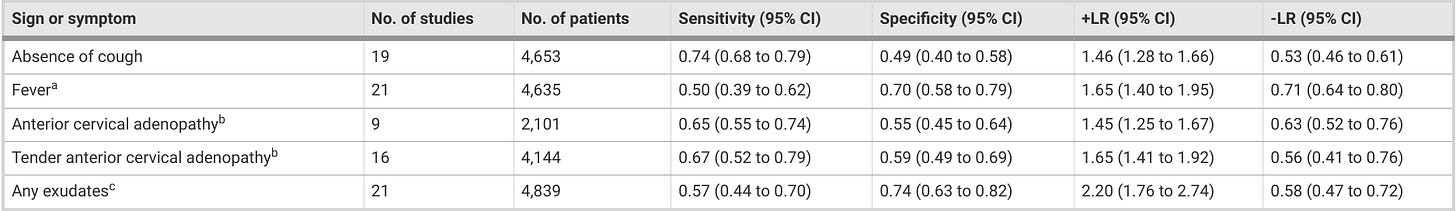
As recently as 2024, a review and meta-analysis found that the Centor criteria are “ineffective at triaging patients who need antibiotics presenting with pharyngitis at hospitals. At high thresholds, too many true positive cases are missed, whereas at low thresholds, too many false positives are treated, leading to the overprescription of antibiotics.”
So the short answer is no.
Unfortunately, using the Centor criteria does not help us differentiate viral from bacterial pharyngitis. We should rely on rapid tests which are 83% (antigen-based) to 96% (molecular-based) sensitive and 99% specific.
—
Dr. Istrail is the author of The POCUS Manifesto: Expanding the limits of our physical exam with point-of-care ultrasound. You can get a copy here.
He is also the author of There’s a Nest in My Chest, a new medical mystery children’s book. You can get a copy here.




