Mosquito Repellents: A Deep Dive
Mosquito bites, DEET, natural repellents, citronella candles, and more.
Dr. Istrail is a physician and author of The POCUS Manifesto: Expanding the Limits of our Physical Exam with Point-of-care Ultrasound
“Blood is life…and it shall be mine”
- Dracula character, Bram Stoker’s Dracula
In the real world, Dracula’s quote and purpose are best embodied by the mosquito. They slurp your blood both to feed their hungry bodies and to expand their family tree. Yet unlike their fictional counterparts, mosquitos that bite people are exclusively female, provide free transport for some of nature’s most ruthless killers, and are not repelled by garlic and sunlight.
More than 500 million people are currently infected with mosquito-borne diseases, and more than 3 million people die every year from these infections. So it stands to reason that safe and effective mosquito repellent could prevent millions from an early demise, and at the very least, make it more pleasant to be outside.
The most deadly of these nuisances of nature is the Anopheles gamiae, the mosquito that carries the malaria-causing parasite Plasmodium. After breeding in the mosquito’s stomach the Plasmodium migrates to the salivary glands where it’s injected into unsuspecting humans’ blood streams in subsequent feeds. They continue their promiscuous mating and mayhem in the host’s liver before entering the red blood cells they eventually destroy in this perpetual cycle that, if untreated, results in the host’s death.

While we have effective treatments for malaria, a strong defense would usurp a potent offense, thus preventing infection and downstream complications in the first place. Like a labrador on the beat of a wounded duck, these tiny, annoying, and lethal insects find their targets with their nose, largely through the compounds and odors that humans excrete. Lactic acid is one attractant. Another is carbon dioxide, which is likely the most potent. Mosquitoes have special neurons with built-in carbon dioxide receptors that, when inactivated, dramatically reduce their host-seeking behaviors. Chemicals that inactivate these neurons would therefore be good mosquito repellent candidates. Yet many prerequisites - notably safety and practicality - must be present for such a candidate to graduate from concept to commercial viability. 2,3-butanedione, for example, inhibits these neurons and deters mosquitos, but its rancid butter odor would also deter pretty girls, and just about everyone else. Ethyl pyruvate, a flavoring agent in food, on the other hand, offers more potential with its caramel/rum odor that mosquitoes don’t care for.
West Nile Virus
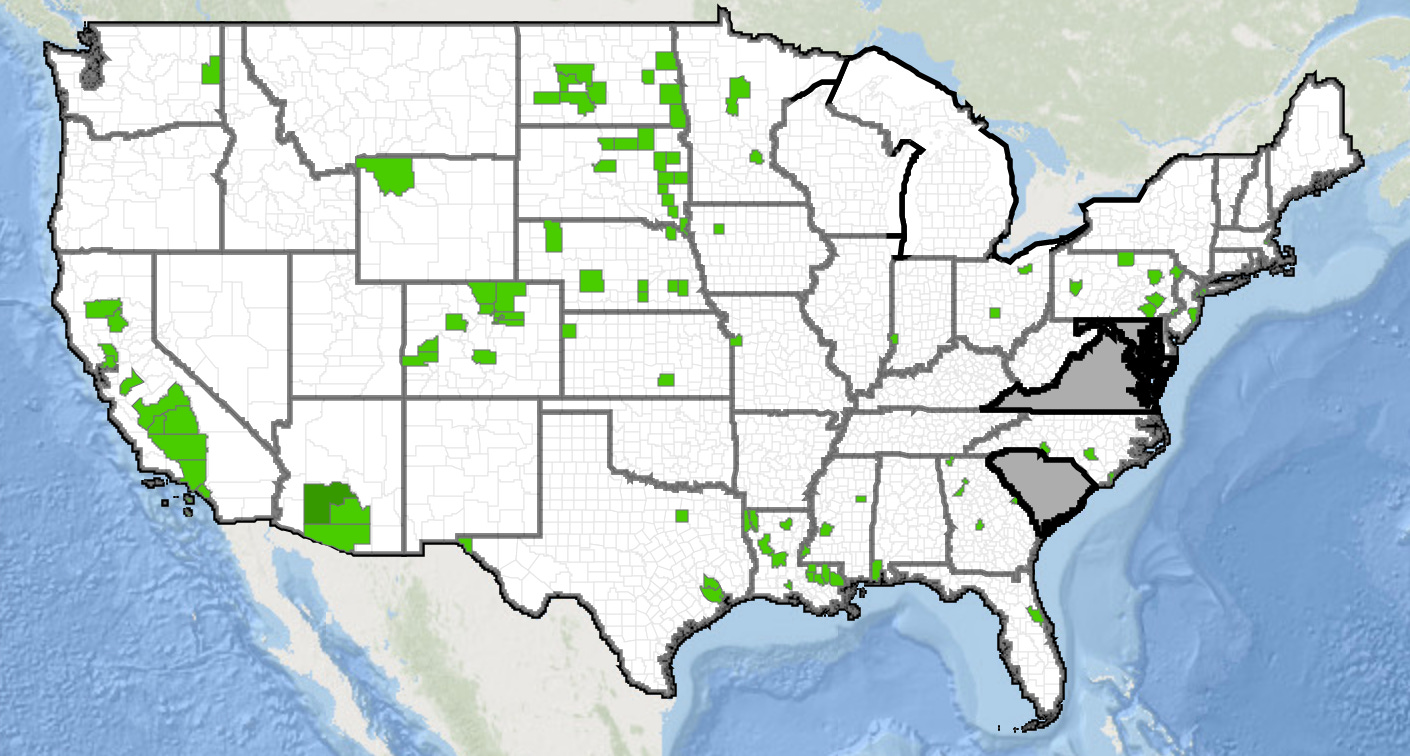
In the United States, the leading cause of mosquito-borne illness is the West Nile virus. By biting infected birds, mosquitoes can become carriers which in turn pass it on to humans with subsequent feeds. Fortunately, most people do not have symptoms, with 1 in 5 developing fevers and only 1 in 150 developing severe disease. Since 1999, Colorado, Texas, and California have had the most cases according to the CDC, ranging from a few cases some years up to 3,000 in Colorado in 2003. In 2020, the most recent year it was recorded, California recorded the highest number of cases with 235, while Virginia, Utah, Oregon, among many other states, were in the single digits. Thus far in 2022, the green areas in the map below represent areas with 10 or fewer cases, while the rest of the country hasn’t reported any.
How Mosquitos Bite
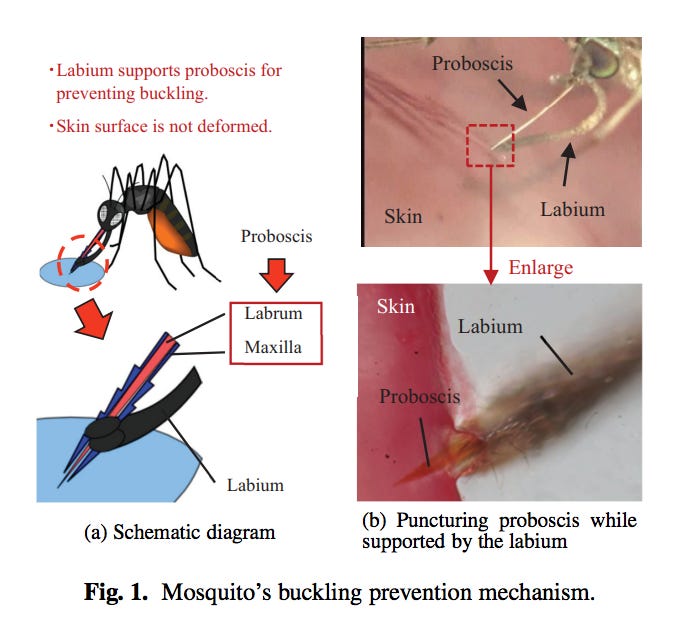
Once they hone in and land on their hairy-human-ankle target, mosquitoes inject their head-hair-diametered proboscis into the skin. It vibrates on entry to dampen discomfort and has a jagged outer surface that minimizes nerve contact, making the whole pain-free arthropod blood draw experience an enviable one. (In fact, these tactics were mimicked by Japanese researchers attempting to create a painless needle for blood draws.)
Once the proboscis punctures the skin, it finds the capillaries and begins the slurp.
To keep the blood flowing, their saliva contains anophelin, an anticoagulant that binds to thrombin, one of the main proteins in the blood clotting cascade, to prevent your blood from solidifying during their meal. Once satiated, they are kind enough to leave you with an immune-provoking parting gift, packaged nicely in their remnant saliva, causing the area to swell and itch.
So how can we prevent them from annoying or killing us?
Repellents
Mosquito repellents fall into three general categories: DEET, picaridin, and ‘others.’ Most in the “others” category don’t work. But notable among them that do offer some deterrence is the lemon eucalyptus extract PMD (discussed later), and Victoria's Secret Bombshell. This commercial perfume is made from a “mix of fresh-cut peonies and exotic fruits in the afternoon sun” that allows you to “float in a cloud” of their signature fragrance. Sounds lovely. But apparently not to mosquitoes.
DEET
DEET, short for N,N-diethyl-meta-toluamide, is a chemical found in most mosquito repellents. It deters them through unpleasant taste and smell, as well as through information garnered through their leg receptors. It has been around since 1957 and its protection time is dependent on the concentration used. A product containing 23% DEET protects for 5-6 hours. At 20% it’s about 4 hours, while 6% concentrated DEET only provides about 2 hours of protection.
Safety
Overall, DEET is generally thought to be safe. At commercial concentrations, one study found that 5% of it was absorbed into the sublayer of skin (the dermis) and that most of the absorbed dose was excreted in the urine within 24 hours. This is consistent with EPA reviews from 1998 and 2014 that did not detect any large safety concerns. A study in pregnant women found “no adverse neurologic, gastrointestinal, or dermatologic effects … observed for women who applied a median total dose of 214.2 g of DEET per pregnancy.” It was detected in the placenta 8% of the time, however, no adverse effects on survival, growth, or development were noted one year after birth.
This was echoed by A New England Journal of Medicine review, which wrote that:
DEET is far less toxic than many people believe. Adverse effects, though documented, are infrequent and are generally associated with gross overuse of the product. The risk of DEET-related adverse effects pales in comparison with the risk of acquiring vector-borne infection in places where such diseases are endemic.
In 20,764 cases of DEET accidental exposure reported to poison control between 1993-1997, the majority reported no symptoms. Those with moderate symptoms were usually managed at home, though some needed hospitalization and some further needed intensive care.
Yet the neurologic concerns are not unfounded.
Ingestion of DEET can cause seizures, severe hypotension, or death. When applied to the skin, there have been reports of severe adverse reactions as well, though in adults this was usually with high concentration products. One of the two reports to poison control that resulted in death was a 26-year-old male applying a high concentration (52%) of DEET and had a seizure and cardiac arrest 10 minutes after application.
In another dramatic case, a 42-year-old woman touched a friend who had just sprayed himself with DEET. The woman “had a habit of touching her face and lips with her hands,” and this resulted in an anaphylaxis reaction, with rapid onset of nausea, angioedema, and loss of consciousness that resolved with epinephrine, steroids, and Benadryl. In another odd case, a man was using DEET daily followed by “a 1-2 hour period in a light-bulb heated box” which resulted in acute manic episodes requiring hospitalization. DEET metabolites were detected in the urine more than 2 weeks after the last application.
In kids, however, even low concentration DEET has caused serious issues. A case series profiled 18 children between 3-11 years old with DEET-induced neurologic complications. Thirteen were exposed through skin application, the majority with low concentration DEET, and three of those unfortunately died.
Regardless of how rare these neurological complications may be, it is a synthetic chemical that some people just don’t feel comfortable spraying on their skin every day.
Picaridin
Picaridin is a synthetic compound available in Europe since the 1990s (as Autan and Bayrepel) and in the United States since 2005. It is as effective as DEET and offers improvements with its lack of chemical odor, lack of damage to clothing or plastics, and likely better safety profile. The exact way it deters mosquitoes is unknown but it is noxious to their taste and olfactory senses and, at 20% concentration, provides about 6 hours of protection, similar to DEET.
Safety
Overall picaridin appears to be safer than DEET. It has been used for over 20 years in Europe, and animal studies have not demonstrated developmental toxicity. In one study, researchers applied high doses to rats daily for two years and did not find any increased risk of cancer. According to the European Chemicals Agency, picaridin has low acute toxicity, and there have been no reported neurotoxicity issues as with DEET. It is not irritating to the skin and only slightly to the eye. It is not recommended by the manufacturer for kids under 2 years old, though there were no developmental, mutagenic, or carcinogenic effects seen.
Between 2000 and 2015, about 1300 cases of picaridin exposure were reported to the United States Poison Control. Of those, the majority (93%) were managed outside the hospital and there were no reported major effects or death.
PMD (para-methane 3-8, diol)

Out of the “others” category, PMD is by far the most effective. It was isolated from the leaves of the lemon-scented gum tree of eastern Queensland, Australia. It was first discovered as part of a 1960 Chinese screening project to discover plants with mosquito repellent properties. With modern formulations to reduce the volatility and increase the protection time, PMD repellents have outperformed low concentration ( < 20%) DEET products and are about equal to high concentration ones. In one California study involving a 6-hour field challenge on 20 participants, the PMD and DEET reduced the mosquito bites by 99.8-100% compared to the control arm with no protection that received more than 1,000 bites! These incredibly impressive results can be seen below with the Repel OLE being PMD and DW Off! being DEET:
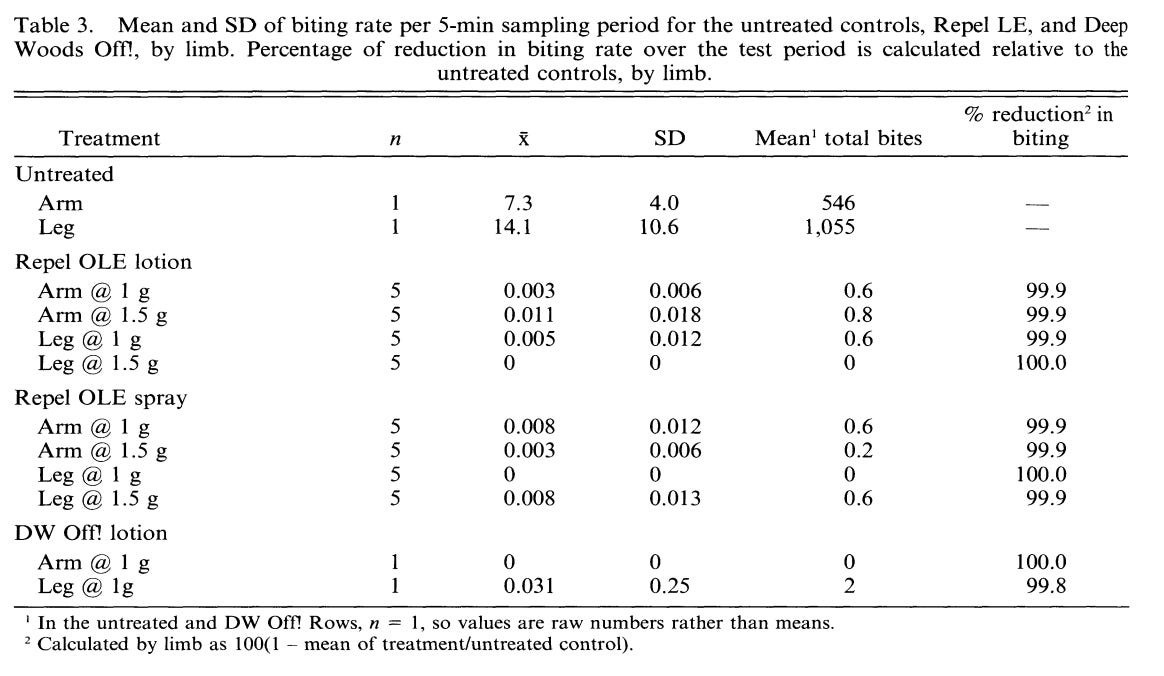
This is similar to a field study in Bolivia in which “the eucalyptus-based repellent containing 30% [PMD] applied at a dose similar to those used in practice gave 96.89% protection for 4 h,” compared to 84% protection with DEET. Similar protection was seen in a 1996 British study which found that “the duration of effective protection for PMD once applied to the skin was very similar to that afforded by DEET.”
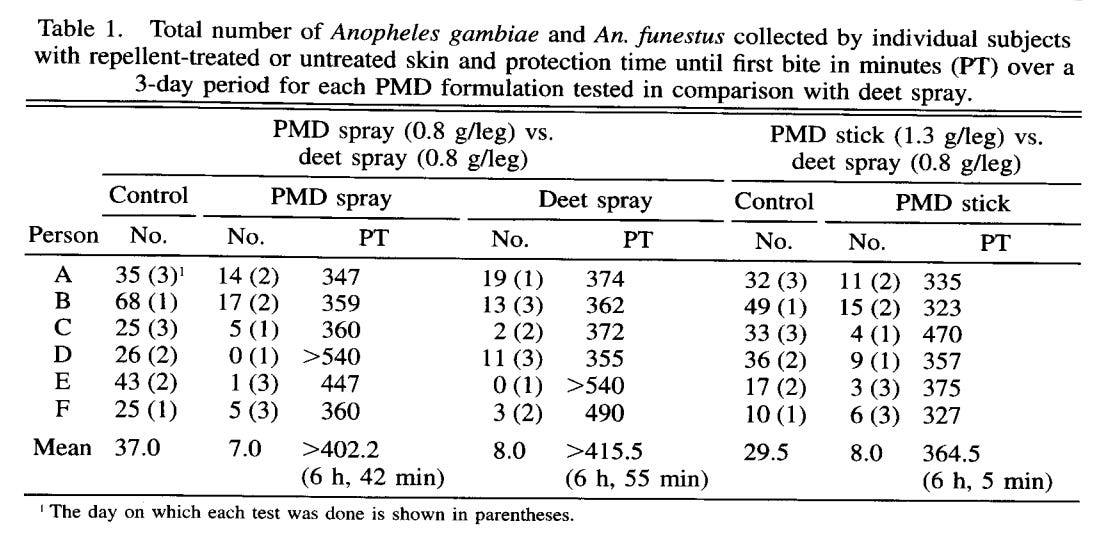
This was consistent with yet another study in Tanzania where 6 subjects sat on the same bench during peak mosquito feeding time. Two had PMD on, two others had DEET, and the third two poor souls had nothing. Compared to the control group that was bitten within 37 minutes with no protection, the PMD provided 6 hours and 42 minutes of protection on par with the DEET spray. They concluded that “PMD is an effective alternative to DEET with potential as a means of personal protection against mosquito vectors of disease.” (Table 1 below)
PMD is commercially available as REPEL, and it earned very high praise from Consumer Reports as the best DEET-free repellent, as well as “one of the best-performing of any that [Consumer Reports] has tested, DEET-containing products included:
With 30 percent oil of lemon eucalyptus as its active ingredient, it earns an Excellent rating for protection against mosquitoes and ticks. Plus, CR’s testers found that, unlike many insect repellents, this product tends not to damage fabrics or other materials.
Apart from mild eye irritation if sprayed in the eyes, PMD does not appear to cause any harmful effects to humans or to the environment according to an EPA review. The CDC does not recommend it for children under 3 but does not give any reasons why, presumably so they don’t accidentally rub it in their eyes.
Repellent candles: Citronella and Geraniol
In addition to spraying your exposed skin, many products on the market claim to prevent mosquitos simply by having them in close proximity. Most commonly these are citronella based candles or incense.
A 1996 study from Canada tested this hypothesis, using 3% citronella candles and 5% citronella incense. They compared these to plain unscented candles and no candles, placing two of each candle or incense at various positions in a wooded area as 8 subjects sat in each of the positions for 8 different nights. The subjects next to the citronella candles received 40% fewer bites compared to the other groups but they still had a significant amount of bites in each group. In an Israeli study of 5% citronella candles, they found that if the candles were 3 meters away they only deterred 12% of mosquitoes and only improved to 15% with the candle 1 meter away. In comparison, geraniol candles performed much better, repelling 70% at 1 meter and 52% at 3 meters. These results were confirmed in an indoor study which showed that the geraniol candles were 5 times more effective than citronella, repelling 85% of mosquitoes.
In a follow up study from 2009, researchers found that when indoor, the citronella and geraniol candles repelency rate was 14% and 50% respectively, while in diffusers it improved to 68% and 97% respectively. When outside, citronella diffusers 6 meters from mosquito traps repelled 58% of female mosquitoes while geraniol deterred 75%.
In summary, there are many highly effective mosquito sprays and deterrents on the market. While they all appear to be safe, PMD and picaridin have less reported adverse effects and are equally effective making them better choices. Citronella doesn’t offer much protection, yet geraniol does. So when having a picnic in peak mosquito season, consider spraying your exposed skin with PMD and surrounding your picnic table with geraniol diffusers to send a strong message to the hungry mosquitoes targeting you: find another human to bite.
-
Dr. Istrail is a physician and author of The POCUS Manifesto: Expanding the Limits of our Physical Exam with Point-of-care Ultrasound